3DCRT is now a very common in radiation therapy as beams are shaped by the MLC to closely fit the area of the cancer.
Radiation Therapy Treatments
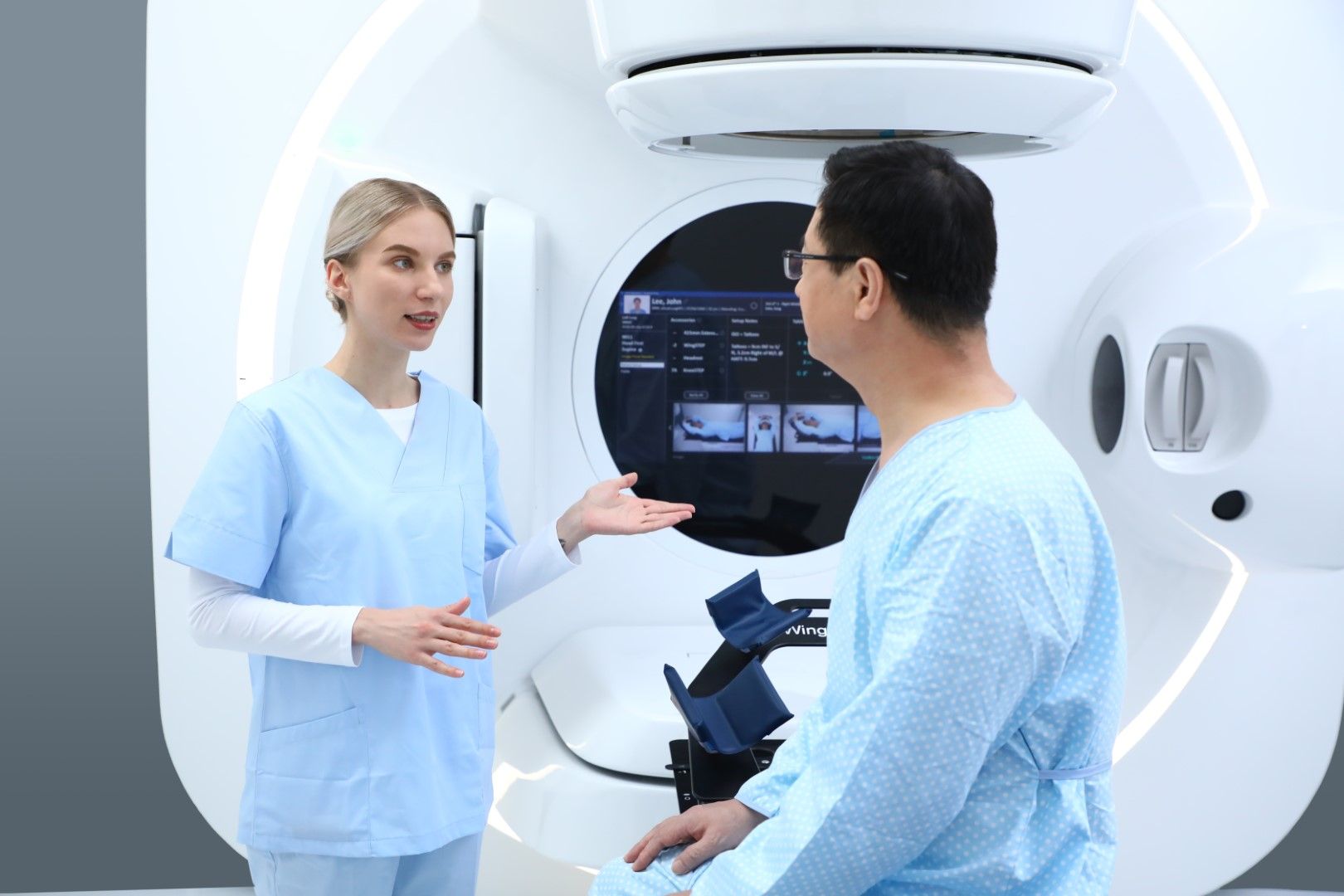
What is radiotherapy and how does it work?
Radiation Therapy or Radiotherapy is the delivery of high intensity X-rays, generally used in the treatment of cancers and brain disorders. There are many ways to have radiation therapy, but they all work in a similar way.
Carefully controlled high-energy X-rays kill or damage cancer cells. This stops them growing or slows their growth. It does this by damaging the cancer cell DNA. Cancer cells whose DNA is damaged beyond repair stop dividing or die. When the damaged cells die, they are broken down and removed by the body.
The aim of RT is simple – to destroy cancer cells, leaving normal healthy cells as unaffected as possible.
Cancer cells are more vulnerable than healthy cells and we exploit this by splitting RT into a number of treatment sessions or fractions. Delivering a small fraction of the total dose allows time for normal cells to repair themselves between treatments, thereby reducing side effects. The total number of treatment sessions that a patient will need is tailored to the treatment requirements of the cancer type.
Radiotherapy is most often given externally by External Beam Radiation Therapy (EBRT), but it can also be given internally with something called Brachytherapy. Internal radiotherapy means having radiation treatment from inside the body.
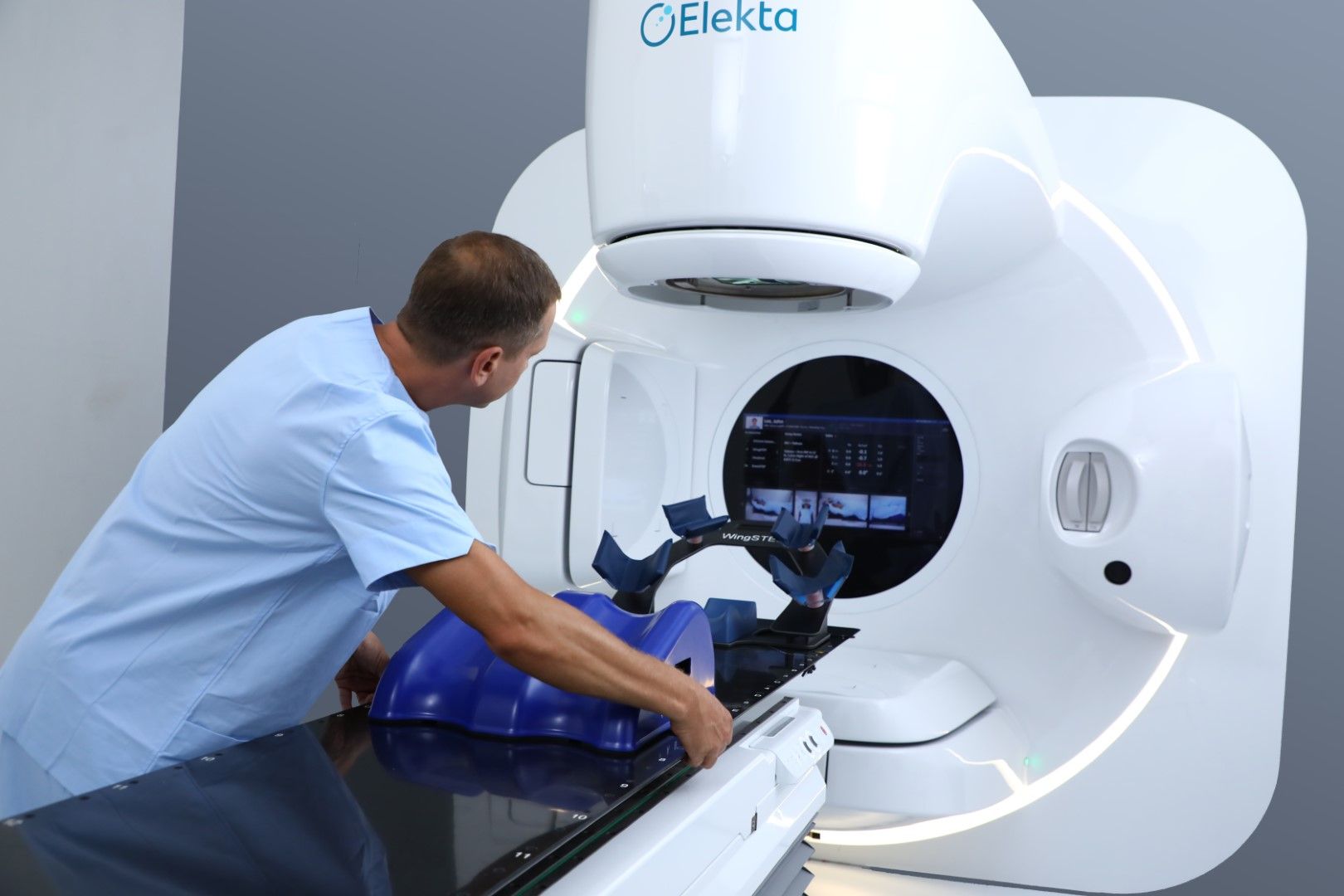
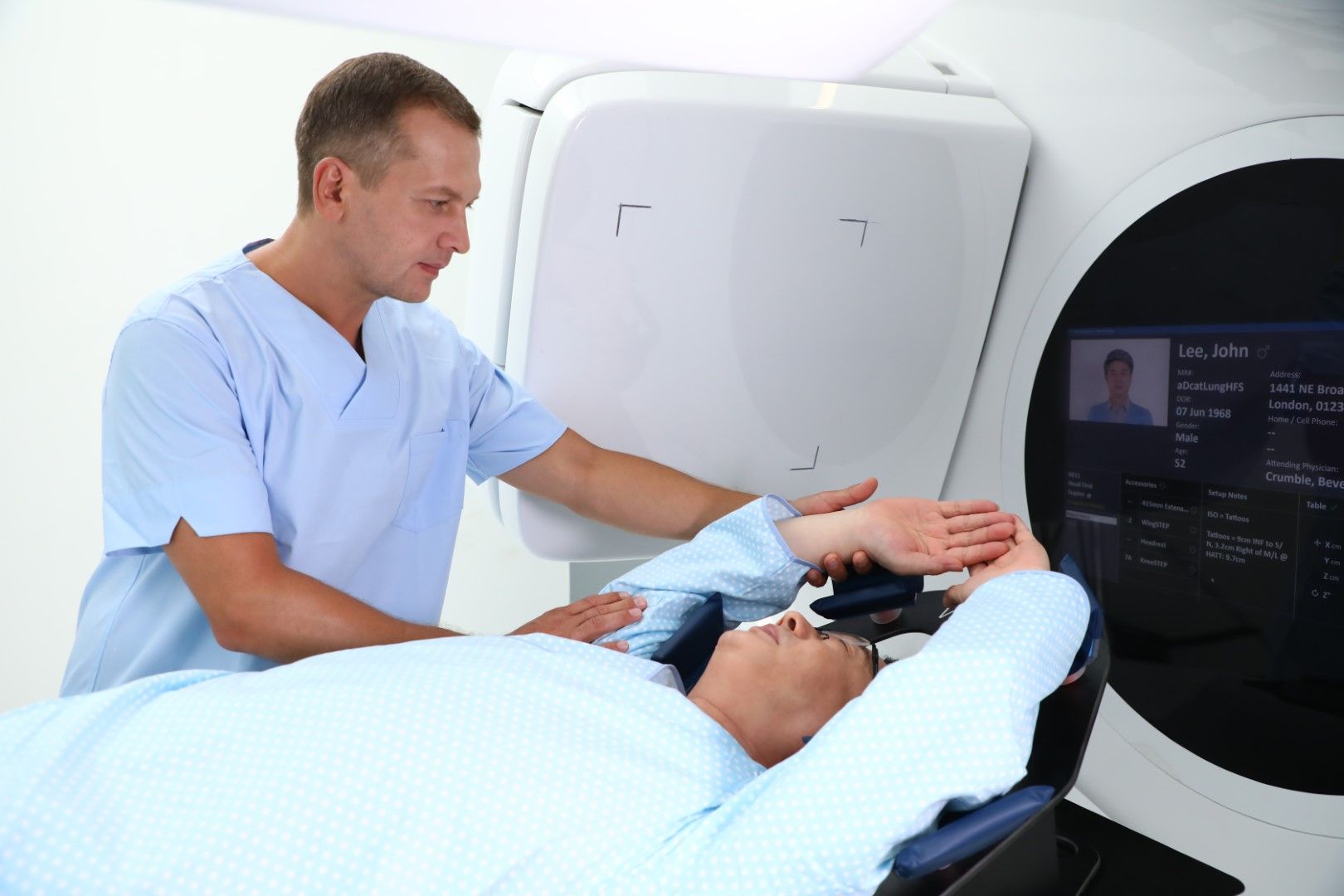
When is Radiation Therapy used?
Every person's radiotherapy is tailored to their unique body, the type of cancer that they live with, as well as the aim of their therapy. Radiation therapy can be intended to cure cancer, but it can also be used to control cancer as well as relieve those cancer-related symptoms that patients may be struggling with.
Radiotherapy is often an adjuvant treatment to other therapies such as chemotherapy and surgery. Sometimes Radiation Therapy it is used as a ‘backup’ to ensure there are no microscopic cells remaining after surgery and chemotherapy, which for example, is often the rationale for whole breast radiation. Sometimes RT is used to shrink a tumor so that surgery can then be performed, for example in some instances of rectal cancer.
What's it's role?

How does it work?

Types of Radiotherapy
External Beam Radiation Therapy
External beam radiotherapy uses a machine outside the body to direct radiation therapy beams at disease, most often cancer, to destroy it. The most common type of machine is called a linear accelerator (Linac), which uses electricity to create the radiation beams. During external beam radiation therapy, a machine moves around you and directs beams of radiation to specific points on the body. The Linac has a device called a multileaf collimator (MLC). The MLC is made up of thin leaves of lead which can move independently. They can form shapes that fit precisely around the treatment area.
The beams are customized to shape the tumor and to protect the patient’s surrounding healthy tissue as much as possible. External Beam Radiation Therapy passes through the body, so it will never make patients radioactive.
Types of external beam radiation therapy
Most types of radiotherapy treatments use photons (such as x-rays), but tiny particles called electrons and protons can also be used.
Photons can treat cancers that are deep inside the body or those on or close to the skin (superficial cancers). Electrons are only used for superficial radiotherapy to the skin.
Treatments using photons and electrons will vary slightly but the experience of having radiotherapy will be similar.
Clinician will choose the type of radiotherapy and the machine for treatment according to the type of cancer and where it is in the body. There are different types of external beam radiation therapy treatment. They include:
3D Conformal radiotherapy (3DCRT)
Image guided radiotherapy (IGRT)
The Linac machines have specialised imaging equipment on-board that can take high-quality X-ray or CT images while patients are on the radiation therapy treatment couch, before, and sometimes even during treatment. These images are compared with the images used to plan your radiation therapy treatment. The clinical team can then make millimetre adjustments to the position of the treatment beams. This ensures that treatment is being delivered very precisely.
Intensity modulated radiotherapy (IMRT)
IMRT is a form of 3DCRT where the MLCs can move while the machine moves around the patient. This shapes the beam of radiation to the tumour and means that the tumour can receive a high dose of radiation and normal healthy cells nearby receive a much lower dose. Each radiation therapy beam is divided into many small beamlets that can vary the intensity of radiation. This allows different doses of radiation to be given across the tumor. This can be very helpful in complex treatment areas where doctors want to avoid critical organs.
Volumetric Modulated Arc Therapy (VMAT)
VMAT is an advanced form of IMRT, where the radiation dose is also varied throughout radiation therapy treatment, but it delivers a continuous beam of radiotherapy in an arc
Stereotactic radiotherapy (SRT) - SBRT SABR
There are a few different terms for stereotactic radiotherapy, which can be confusing. Stereotactic treatment for the body can be called stereotactic body radiotherapy (SBRT) or Stereotactic ablative radiotherapy (SABR). All these terms describe a non-invasive, advanced radiotherapy technique that targets tumours using highly focused beams of radiation and shorter treatment schedules to destroy cancer cells with minimal damage to surrounding healthy tissues. This can be used to treat localised tumours (where the cancer is only found in the tissues where it started) or to delay the growth of tumors that have spread to other parts of the body.
Radiosurgery (SRS)
Stereotactic radiosurgery (SRS) is a non-surgical radiation therapy used to treat small tumors of the brain and functional abnormalities. It can deliver precisely-targeted radiation in fewer high-dose treatments than traditional therapy, which can help preserve healthy tissue. When SRS is used to treat body tumors, it's usually called stereotactic body radiotherapy (SBRT).
Adaptive radiotherapy
Describes a type of radiotherapy where treatment is adapted to account for internal changes to a patient’s anatomy as some organs in the body that need radiation therapy can change in size, shape and position.
MR guided radiation therapy
a type of radiotherapy guided by MRI (magnetic resonance imaging) that offers more options adaptive radiotherapy with real-time imaging and aims to reduce treatment sessions and side effects.
Hypofractionated radiotherapy
means more doses of radiation are delivered per treatment, so patients can complete their course of radiation therapy much faster than conventional treatment. Some patients may be eligible for extreme hypofractionation with SBRT (stereotactic body radiation therapy), which, when appropriate, can shave weeks off the traditional treatment length.
Brachytherapy (Internal Radiation)
Brachytherapy is a procedure used to treat certain types of cancer and other conditions. It involves very precisely placing radioactive material inside the body using special devices. This is sometimes called internal radiation and means a large dose of radiation can be delivered straight to or by the tumor. There are different types of brachytherapy, sometimes a radiation source can be implanted straight into an organ during surgery. Most often, brachytherapy is given using radioactive sources enclosed in special protective capsules. These then travel through applicators to the part of the body requiring treatment.
The two main types of brachytherapy, high dose rate brachytherapy and low dose rate brachytherapy, depending on the type of cancer you have.
High dose rate brachytherapy
One of two types of temporary brachytherapy. The radioactive material delivers a high dose of radiation to the tumor in a short burst, lasting only a few minutes. This treatment may be repeated several times in a day or a number of times over one or more weeks.
Low dose rate brachytherapy
LDR brachytherapy is a type of radiation therapy that involves placing a small, (medically safe) radioactive pellet or seed that releases radiation directly into a tumor over several days.