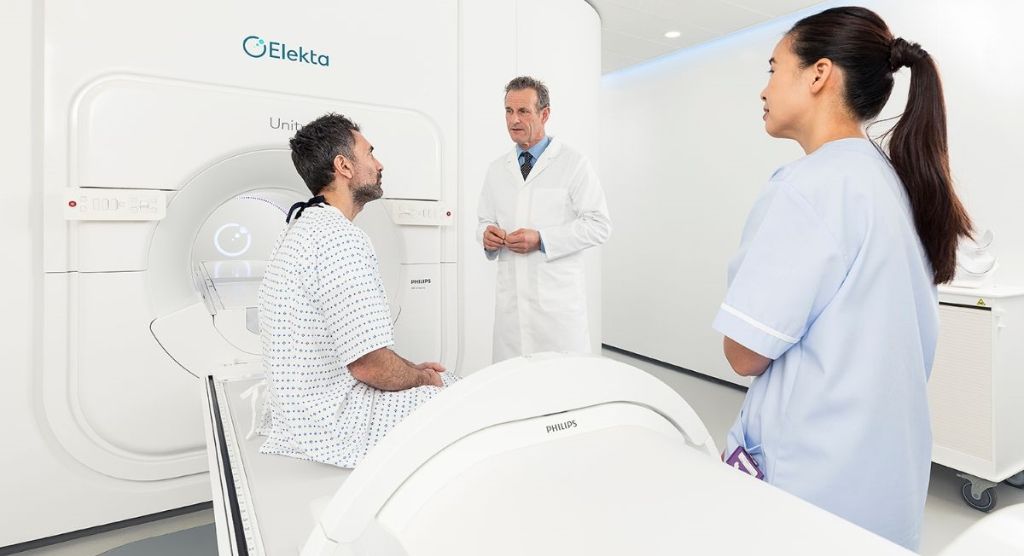
Washington state center harnesses C-RAD technology to enhance patient setup and motion monitoring

Seattle Cancer Care Alliance South Lake Union implements Surface Image Guided Radiation Therapy

An effort spearheaded by physicists at Seattle’s Washington’s Seattle Cancer Care Alliance (SCCA) South Lake Union (Seattle, Washington) led to a more streamlined, integrated solution for patient positioning and motion management. In early 2017, the center implemented C-RAD’s Catalyst HD system to enable Surface Image Guided Radiation Therapy (SGRT), a non-ionizing imaging technique to guide patient positioning during setup, monitor intra-fraction motion and guide gated treatment deliveries.
The team selected the C-RAD Catalyst HD system for SGRT (see sidebar: What is SGRT?) because of its seamless integration with the clinic’s Elekta linacs and MOSAIQ® Oncology Information System. It could also be used for both simulation and treatment, allowing the clinic to have a single system throughout the patient journey.
SCCA’s previous method for breath-hold treatments involved using two different patient motion management systems for simulation and treatment. This required the transcription and translation of data between the two systems, which was time-consuming and cumbersome.
“Using the single C-RAD Catalyst system to deal with all the information rather than two separate systems is far preferable.”
“Using the single C-RAD Catalyst system to deal with all the information rather than two separate systems is far preferable,” says Juergen Meyer, PhD, Clinical Physics Lead at SCCA South Lake Union. “The C-RAD system provides a more integrated, efficient workflow and offered some unique features that influenced our decision, such as its ability to project information onto the patient and the quality of the deformable registration algorithm it uses.”
The C-RAD systems were installed in SCCA South Lake Union and University of Washington Medicine Center (UMWC) Northwest in 2016. In February 2017, following physicist and therapist training, implementation began using a phased approach designed to build confidence in the new method and to ensure a comfortable transition for the radiation therapists.
“SGRT implementation was a team effort for us,” Dr. Meyer says. “Initially, the physics team drove it in close collaboration with the chief therapist. SGRT champions were allocated for each machine to help get everyone on board, and then the radiation therapists drove the advanced implementation stages, based on their comfort levels and the clinical utility of the technology.
“As soon as we started to experience the benefits of the new system, everyone was very happy with the change,” he adds. “We did much of our learning by doing, but a SGRT task group [TG302] has been established to provide guidelines that will hopefully expedite implementation for others.”
Phased implementation
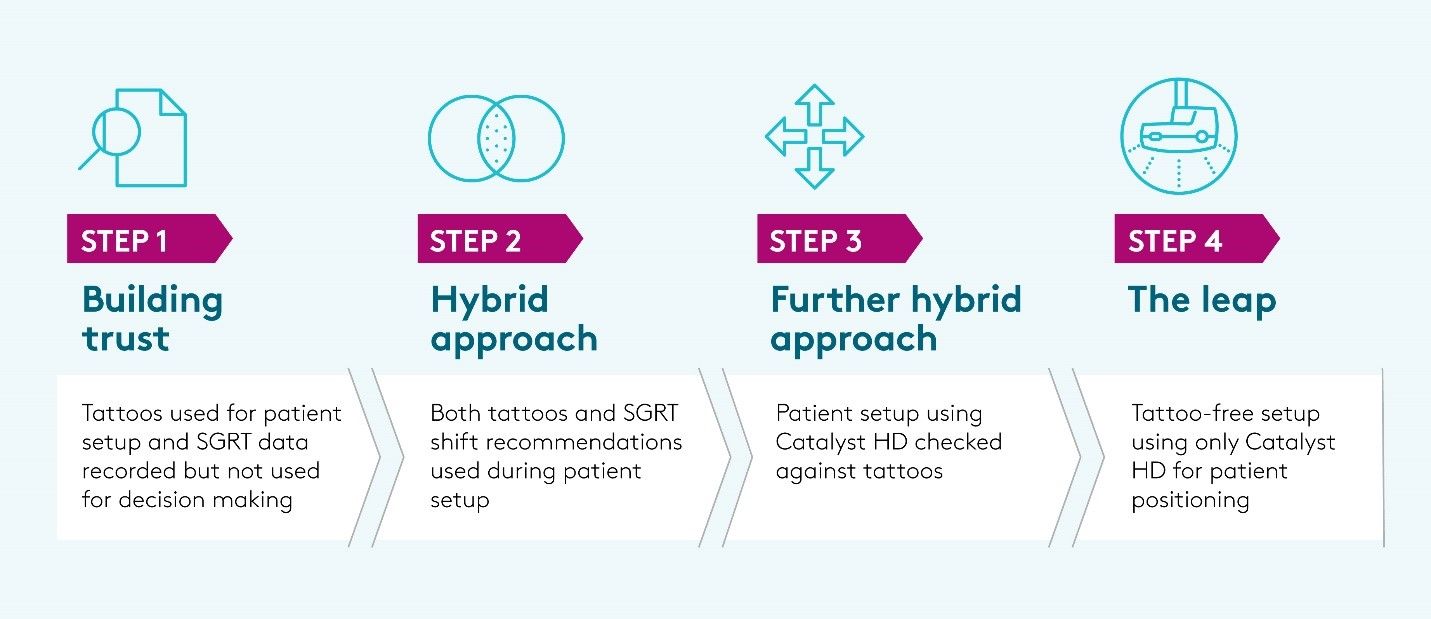
SCCA’s C-RAD implementation steps entailed building trust, a hybrid approach, further hybridization and “the leap” to use C-RAD by itself.
SGRT setup workflow
The VSim starts with a sternal reference instead of going straight to the isocenter (ISO) reference. Since the C-RAD algorithm weights the isocenter heavily, it was found that the sternal reference provides the most accurate setup for visualizing rotations. Patients are very accurately lined up with the sternal reference (within 1 mm, 1°) and then the nominal shifts to ISO are applied. The C-RAD Catalyst shifts are displayed and checked before they are applied. If the rotations are out of tolerance, or if orthogonal pair imaging shows that shifts are required, then a new reference image is acquired.
“In the beginning, images were obtained for three days when a new reference image was captured to check that everything was OK,” says SCCA South Lake Union radiation therapist Chris Norris. “This was reduced to two days because we are consistently setting up patients very accurately using SGRT.”
“We achieved significantly higher positional accuracy and improved precision with the C-RAD Catalyst HD system.”
SCCA uses SGRT technology to guide patients during a deep inspiration breath hold (DIBH) for left breast radiotherapy.
“We predetermine the required breath depth during simulation and planning,” he says. “We can then reproduce this breath hold precisely during treatment, using a virtual tracking point on the patient’s sternum and audio-visual feedback to the patient. When we conducted a study to evaluate the accuracy and stability of DIBH using SGRT compared to our previous radiofrequency transponder method, we achieved significantly higher positional accuracy and improved precision with the Catalyst HD system.”3
Integration with Elekta linacs ensures an efficient, streamlined workflow for patient positioning and motion monitoring, as well as automatic treatment gating for DIBH treatments using Elekta’s Response gating interface.
Workflows transformed with SGRT
“Our main motivation for adopting SGRT was for breast patients,” Dr. Meyer notes, “but in principle, SGRT could be used for all patient setups. For example, we find it particularly helpful for prone patients, to correct any posture changes prior to CBCT imaging.
“SGRT has transformed our workflows, improving efficiency and enhancing setup accuracy.”
“There is an initial investment to implement SGRT, but it has transformed our workflows, improving efficiency and enhancing setup accuracy,” he continues. “Building staff confidence during implementation was really important for maximum uptake in the clinic. When the therapists see the information SGRT provides, it gives them the confidence to use it in different situations.
“SGRT continues to develop with the introduction of new features, such as collision avoidance and patient identification,” Dr. Meyer adds. “These developments make good use of the technology and will further impact patient safety in the years to come.”
Learn more about SGRT, or contact your local Elekta representative.
What is SGRT?
Precise patient positioning during setup and radiation dose delivery is critical in radiation therapy, as anatomical deformations and posture variations can impact the position of internal anatomy1.SGRT uses optical technology and cameras to obtain real-time 3D information about the patient’s surface. This live surface image is compared to a reference image of the desired treatment position, obtained during CT simulation. Surface image registration is then used to verify that the patient is in the correct position or if any part of their body has moved out of position. Since the surface contour of the patient is only a surrogate for actual tumor position, surface registration algorithms are used to calculate any required isocenter shifts during setup.1
Complementing x-ray-based 2D and 3D image guidance systems, SGRT can be used daily as it doesn’t use ionizing radiation to obtain real-time 3D patient surface information. Compared to three-point localization and benchmarked against cone beam CT, surface imaging has been shown to improve patient setup accuracy considerably. In a retrospective analysis of over 6,000 fractions, three-point localization resulted in average shift magnitudes of 0.9 – 1.4 cm for different anatomy sites, whereas the average magnitude of SGRT-based shifts were 0.5 – 0.6 cm.2
Advantages of SGRT
Accurate patient setup
A UWMC Northwest retrospective study compared three-point localization with SGRT for patient positioning during setup. The study recorded the number of times additional shifts were required following orthogonal pair imaging. Three-point localization required additional shifts 18 percent of the time, while SGRT required shifts just eight percent of the time – a significant decrease.By setting up patients more accurately, SGRT requires fewer shifts and less imaging, resulting in faster treatment setups and less imaging dose to the patient.
Workflow efficiencies
Workflow efficiencies are achieved through system integration in the Elekta environment; by eliminating the need for transcription and translation of data; by removing post-simulation tattooing; by requiring fewer shifts and less imaging during patient setup; and by reducing setup note adjustments.Visualizing anatomical changes and rotations
SGRT is excellent at identifying anatomical changes, such as weight loss, swelling, a deforming breast implant or a moving tissue expander. Such rapid evidence of tissue changes without the need for further imaging ensures faster decision-making.“We had a patient whose expander had shifted laterally prior to VSim,” Norris recalls. “We could see the difference right away when we began patient setup, without needing to obtain x-ray images. We were able to consult the physician and physicist immediately, and to obtain another simulation scan with minimal delay.”
Unlike the clinic’s previous method for patient positioning, SGRT is also able to detect rotational errors during setup.
“During our evaluation period, we compared SGRT to three-point localization in a right breast patient,” Dr. Meyer observes. “On Day 19 of a patient’s treatment, the Catalyst HD system detected a pitch error that we couldn’t see with the previous method. This convinced many people of SGRT’s value and provided the motivation to push forward with implementation. You don’t know what you can’t see and what you see you can’t unsee.”
“In general, SGRT also complements CBCT by allowing us to correct rotational errors during patient setup, prior to CBCT imaging,” he explains. “Since adopting SGRT, we can now tighten our rotational tolerances so that we don’t proceed to the next step until they are within 1° [2° maximum].”
Enhanced safety
Monitoring the patient using SGRT before and during treatment ensures that radiation is not delivered if the patient has moved out of position, thus ensuring accurate dose delivery and enhanced patient safety.“SGRT enhances our confidence by allowing us to see information that we didn’t see before,” Dr. Meyer says. “If a patient coughs, for example, and moves out of position when you leave the room, you may not realize it happened, but SGRT detects it and alerts you to it. You can then see if the patient has moved back into position before you proceed or if the patient needs to be set up or imaged again.”
References
- Meyer, J, Smith, W, Geneser, S. (2020) Characterizing a deformable registration algorithm for surface-guided breast radiotherapy. Med. Phys. 47 (2): 352-362.
- Stanley, DN, McConnell, KA, Kirby, N et al (2017) Rad Onc Phys. Comparison of initial patient setup accuracy between surface imaging and three-point localization: A retrospective analysis.
- Kalet, AM, Cao, N, Smith, WP. (2019) Accuracy and stability of deep inspiration breath hold in gated breast radiotherapy – A comparison of two tracking and guidance systems. Physica Medica 60: 174–181.