Elekta Unity MR-Linac reflects radiotherapy department’s image

University of Iowa closes in on first year of MR-guided radiotherapy

Leaders at the University of Iowa’s Department of Radiation Oncology (Iowa City, Iowa) had a vision more than 15 years ago to inject as much imaging technology into their service as possible – limitations in their ability to visualize tumor targets were no longer acceptable. So, in 2005, the University of Iowa (U of I) established a brand-new radiation oncology facility and adopted the name The Center of Excellence in Image Guided Radiation Therapy. The center went live with a 3.0T MRI system, a 40-slice respiratory-gated PET-CT scanner as its standard simulator and made sure all its linear accelerators were equipped with cone beam CT and optical guidance systems.
“Since then, our clear focus has been on quantitative imaging applications to radiation oncology and the application of high-end, exquisite imaging to the treatment planning process,” says John Buatti, MD, chair of the Department of Radiation Oncology. “As we moved forward, we viewed Elekta Unity as a natural, key piece of equipment that is totally consistent with our departmental focus and with our research interest in applying quantitative imaging for therapy.”
While Elekta Unity is not the only MR-Linac commercially sold, it is currently the first and only high field (1.5T) system available. Dr. Buatti and his colleagues considered the choice of field strength a significant factor in their selection of Unity.
“Because we believe that ultimately we will be able to use some of the functional imaging capabilities of MR-guided radiotherapy we saw the 1.5T field strength as critical,” Dr. Buatti says. “If you want to consider techniques such as arterial spin labeling for non-contrast perfusion-weighted imaging and diffusion-weighted imaging, you really need the speed and signal-to-noise ratio of high field MRI. Acquiring a 0.35T was definitely a non-starter for us from a functional imaging standpoint.”
Better eyes on the target
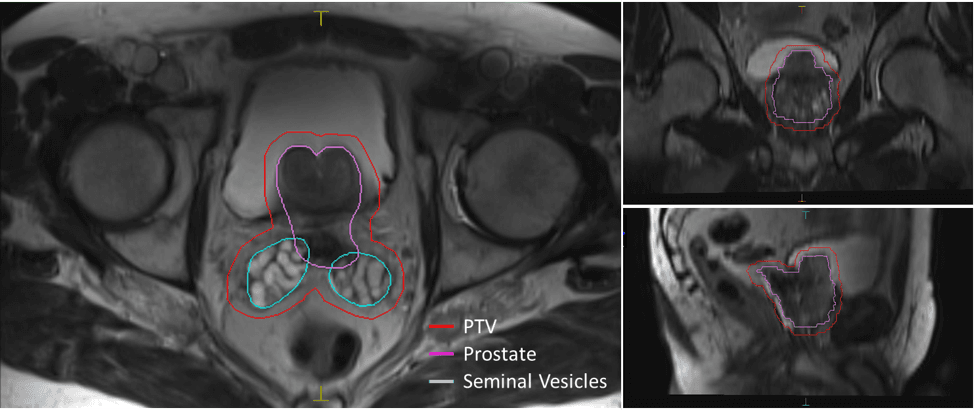
U of I clinicians launched their MR-guided radiation therapy program last May with the treatment of an 80-year-old individual with prostate cancer (Figure 1). The value of Unity for his case was immediately apparent.
“It was eye-opening that on the patient’s very first fraction, the MR images showed that his seminal vesicles were flipped in the opposite direction, so we had to Adapt to Shape [see sidebar] immediately,” Dr. Buatti recalls. “Cone beam CT would not have shown us this, so it was a nice first fraction illustrating the need for the MR-Linac.”
Over the last several months, U of I physicians have treated another 48 patients, encompassing 725 fractions and averaging about 10 patient treatments each day. The most common indication has been prostate cancer, with oligometastatic disease a close second, followed by fewer numbers of cases for tumors in other anatomies, such as the liver and brain.
“The prostates have been a big hit here,” says U of I physicist Daniel Hyer, PhD, MR-Linac Technical Director. “We have two physicians treating those cases and they really appreciate the ability to adapt the therapy each day and they ultimately moved into mild hypofractionation for some of these patients, which was something that we did not do here before Elekta Unity.”
The U of I doctors are following the PRISM Trial fractionation schedule of a 60 Gy total dose delivered in 20 fractions. Traditional prostate radiotherapy entails 39 fractions for a total dose of 78 Gy.
“This has attracted some patients who would be willing to travel a bit further if they are able to have a shorter course of radiation and potentially more accuracy and the ability to account for daily variations in prostate shape and position,” Dr. Hyer adds.
Elekta Unity treatment of oligomets has also been a “big hit.”
“The system has increased clinical confidence because not only can you see these lesions well for daily planning, but you can also monitor their position throughout treatment,” he says. “These are fairly small targets and they’re deep within the soft tissue, so it’s nice to be able to see that you’re getting those throughout the entire course of treatment.”
Margins shrinking
Better visualization of different soft tissues has made it possible to reduce margins in a way that wasn’t possible before Elekta Unity.
“I can very confidently place the treatment isodose line at the interface between the tumor and brainstem and leave virtually no margin.”
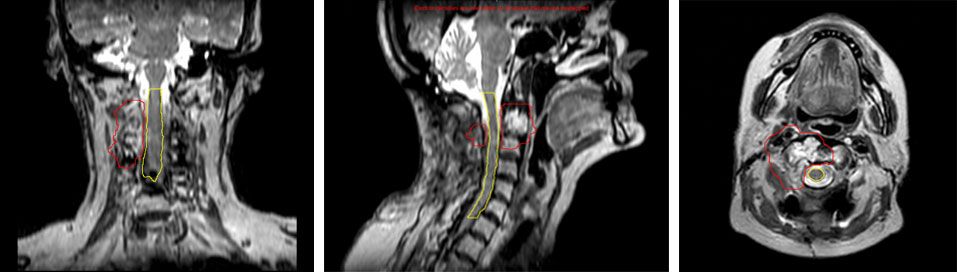
“This has certainly been the case for patients with indications like a chordoma [Figure 2],” Dr. Buatti says. “With Unity, we can actually see the spinal cord and upper portion of the brainstem where it directly abuts the tumor. Previously, I would have to make a PTV margin that excluded the area where I couldn’t discern the dividing line between the two structures. Now, I can very confidently place the treatment isodose line at the interface between the tumor and brainstem and leave virtually no margin or a miniscule margin where I typically had been compelled to leave a three- to five-millimeter margin.”
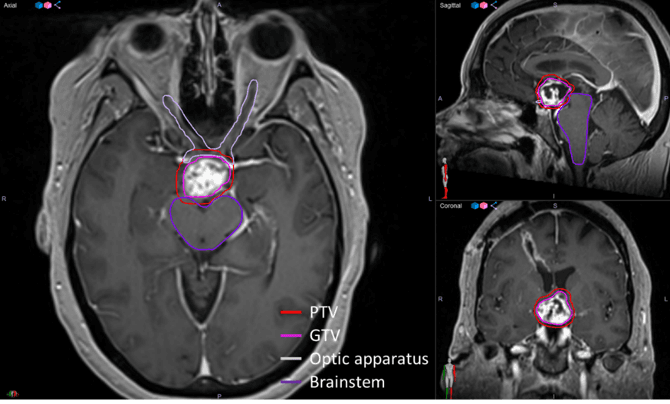
This patient would ultimately receive conventional linac treatment to take advantage of non-coplanar beam arrangements and to reduce the dose to normal tissues. However, since then, the U of I team has treated several brain tumor patients with Elekta Unity, such as the chordoma patient In Figure 2, with very little/no margin between the target and brainstem.
Another recent case in which clear lesion visualization was important was a patient with Ewing’s sarcoma.
“With Unity we could see several soft tissue masses around the gluteal region that were taking on different shapes each day due to compression from sitting,” he says. “I know that if I had treated using CT guidance I might have been aligning to bone, and with CT’s poorer soft tissue visualization I probably would have given it a bigger margin. But with a larger margin I wouldn’t be sure I was treating the target completely. The bottom line is that for the vast majority of cases, if I can see the target better then I will reduce the margins.”
The MR-Linac’s ever-expanding horizon
New opportunities to either modify treatment plans based on a pathology’s functional characteristics or to use MR-guided radiotherapy for indications traditionally treated with other modalities are now on the horizon thanks to Elekta Unity.

“With some gliomas you could look at perfusion and consider alternating the doses based on the tumor’s perfusion parameters,” Dr. Buatti says. “Similarly, for head-and-neck cancers, you know that there are hypoxic regions and we should be able to image those on a daily basis with functional imaging and modify the daily treatment plan accordingly with those types of images. I see cervical cancer as another potential indication for the MR-Linac as well. Most of the boosts are now done with brachytherapy and external beam radiotherapy, but there are occasional patients that require IMRT or can’t tolerate brachytherapy so Elekta Unity could also be deployed for that.”
The integration of respiratory gating for Elekta Unity could also open up new applications for the system, Dr. Hyer adds.

“Respiratory gating could unlock a whole subset of patients we currently aren’t treating or treating less precisely with another system, such as cancers of the mediastinum, liver, lung and kidneys – all mobile targets that could be treated with more robust gating methods,” he says.
“High-field MR-guided radiotherapy is going to end up being the most important paradigm shift in radiotherapy technology.”
“High-field MR-guided radiotherapy is going to end up being the most important paradigm shift in radiotherapy technology,” Dr. Buatti says. “And I think we are still at the very, very early stages of discovering all the potential uses for this technology.”
Learn more about Elekta Unity.
Daily plan adaption options with Unity MR-Linac
MR-guided radiotherapy with Elekta Unity enables two different types of daily plan adaptation: Adapt to Position (ATP) and Adapt to Shape (ATS), both of which permit changes to the therapy that compensate for shifts in target position or treatment-related changes in target shape for each patient. In ATP, the shape and weight of beam segments in the reference plan are adjusted to match the current position of targets and organs-at-risk (OAR) based on rigid registration. In ATS, a new plan is created to match the anatomy of the day using deformable registration for contour propagation from the reference plan to the session MRI, followed by manual adjustment of the contours if necessary.