Elekta template helps Morocco clinic boost prostate brachytherapy success
Martinez Prostate Template Set provides Clinique Spécialisée Menara clinicians with precision needle implantation in HDR brachytherapy
Because a potent, targeted post-EBRT boost of high dose rate (HDR) brachytherapy has been shown to result in a higher prostate cancer control rate than EBRT alone,1-3 the technique has earned an important place in the treatment of eligible high and intermediate-risk patients.

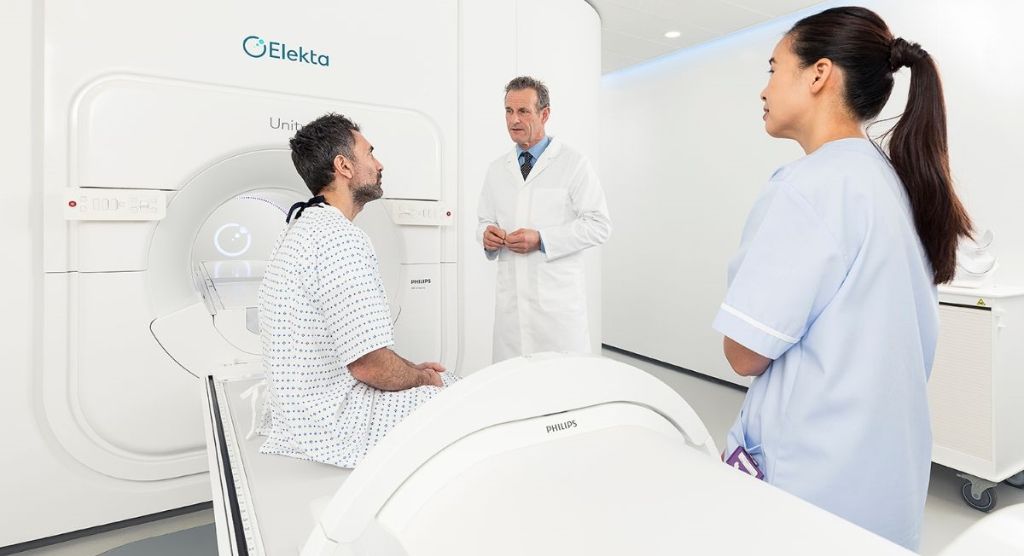
Clinicians at Clinique Spécialisée Menara (Marrakesh, Morocco) began treating these patients with a single-fraction HDR brachytherapy (BT) boost in 2015 after acquiring Elekta’s Flexitron® afterloader, and the company’s Martinez Prostate Template Set, the latter a critical tool to ensure precise, ultrasound-guided brachytherapy needle placement.
“According to the literature, HDR brachytherapy combined with EBRT can increase both disease-free survival and distant metastases-free survival to 90 percent and higher after five-year follow up in comparison to EBRT alone,” says Clinique Menara radiation oncologist Aziz Ammor, MD. “And, because the radiation is highly targeted, reports indicate low rates of late genitourinary toxicity.”
Clinique Menara, the first private clinic in southern Morocco (est. 2013) to diagnose and treat cancer, is also the country’s first medical center to acquire the Martinez template set (Figure 1), a solution that Dr. Ammor considered essential for interstitial brachytherapy of the prostate.
“After researching what was on the market, I really liked the design of the Martinez template.”

“After researching what was on the market, I really liked the design of the Martinez template,” says Dr. Ammor, a veteran BT practitioner with experience at Centre Antoine Lacassagne in Nice, France. “The numbered and lettered grid on the face of the template itself – in addition to the corresponding grid displayed on the ultrasound screen – convinced me that I would be able to very accurately position the needles in the prostate, but especially in the seminal vesicles, for which the Martinez seemed to be better.”
Before implementing the technique for prostate patients, the Clinique Menara team began using their Flexitron® afterloader in 2015 for gynecological cases – patients with cervical and uterine malignancies – and later added patients with prostate and breast cancer (BT boost) and those with keloid scars. Before 2015, Clinique Menara had to send patients who would benefit from brachytherapy to centers distant from Marrakech, presenting transportation difficulties. Since the clinic opened, 350 patients have received EBRT for prostate cancer on Clinique Menara’s two linear accelerators and since 2015, 110 patients have also received an HDR prostate brachytherapy boost.
For its new treatment modality, Clinique Menara formed a multi-disciplinary team (MDT), including a radiation oncologist, medical oncologist, urologist, medical physicist and a surgeon, and will soon add an anesthesiologist.

“In the past, prostate cancer patients consulted first with a urologist, who typically recommended surgery as the frontline option,” Dr. Ammor says. “Now, the MDT meets and discusses the optimal treatment for each patient, which in some cases could be a less invasive alternative.”
The definitive treatment for all patients with intermediate and high-risk prostate cancer is EBRT to the prostate and lymph nodes, with a total dose of 46 Gy delivered in 23 fractions over four to five weeks. This is followed by a single-fraction HDR brachytherapy boost of 15 Gy equivalent dose to the prostate.
“Before we began boosting these patients in 2015, the conventional EBRT dose and fractionation was 78 Gy in 39 fractions, however the biological equivalent dose to the bladder and rectum was about 70 Gy, which was causing unacceptably high toxicity,” he notes. “When we added the HDR boost, we were able to reduce the EBRT dose to 46 Gy. In addition, although we started the brachytherapy boost at 14 Gy, the results were so encouraging that we escalated to the current dose of 15 Gy in the second year.”
Dr. Ammor adds that the single-fraction 15 Gy boost focused only on the prostate has a biological dose equivalent of 100 Gy and higher, while limiting toxicity to nearby OAR.
The selection criteria for patients eligible for HDR brachytherapy boost are fairly minimal; the patient should be in good physical health, the size of the prostate must not exceed 85 cc and the patient’s pelvic size must be amenable to the procedure.
A streamlined, simple workflow
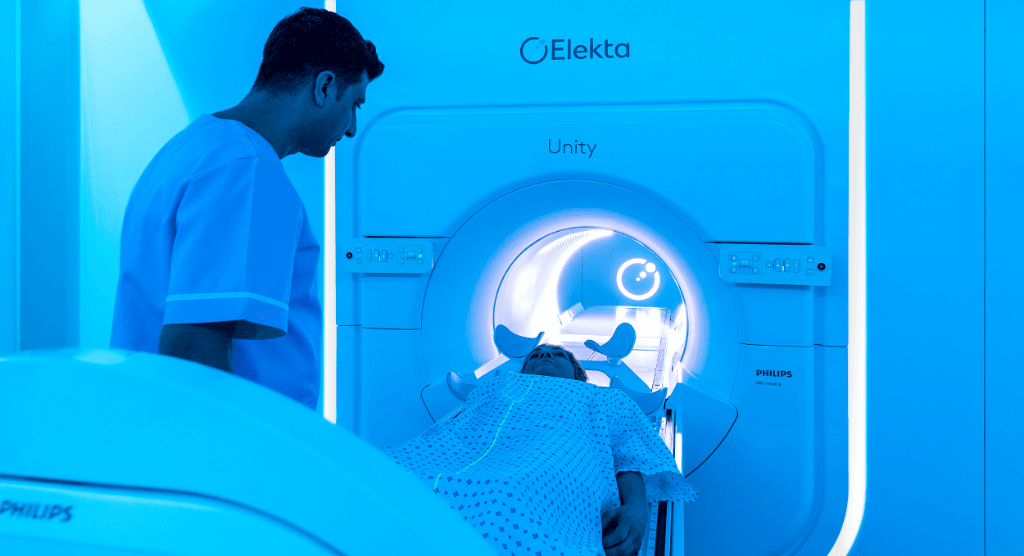
The patient reports to the hospital the day before the procedure to determine the suitable concentration of general anesthesia to administer and to clean the operative area (perineum). On the morning of the procedure, the perineum is again sterilized with antiseptic, a urinary catheter is placed and the patient is anesthetized.

In the operating room, a transrectal ultrasound probe is used to visualize the prostate and OAR and to guide insertion of 17 to 20 plastic ProGuide needles into the gland (Figure 2). Following implantation, the needles and Martinez template are fixed on the perineum and the patient is shifted to the CT room for image acquisition.
“A useful feature on the Martinez template is that during the shift of the patient to the CT room, each needle aperture has its own individual locking insert,” Dr. Ammor notes. “This ensures that the position of each needle will remain unchanged and well-fixed in the prostate with minimal movement.”
The CT images are sent to the Oncentra® Brachy treatment planning system for digital needle reconstruction (Figure 3), followed by contouring of the target and OAR.
“In my view, Oncentra Brachytherapy is a very advanced tool for 3D contouring and image registration.”

“In my view, Oncentra Brachytherapy is a very advanced tool for 3D contouring and image registration,” according to Clinique Menara physicist Abdennacer Ait Ayoub. “The system has rapid and powerful calculation tools and forward and inverse calculation algorithms, enabling a very efficient and precise calculation of the dose distribution for each patient.”
During inverse planning, optimization of source dwell position and dwell time are performed. Dwell time is typically between 20 and 100 seconds, he adds. The total irradiation time is between 10 and 20 minutes.
After these steps, the plan is sent to Dr. Ammor for approval. Once approved, the plan is transferred to the Flexitron treatment console, where each needle is connected to a specific channel determined during plan calculation.
Following treatment delivery, the needles and template are removed and the patient is hospitalized for 24 hours for needle path irrigation.
The entire process usually begins at 9:00 am with treatment starting at approximately 11:00 am. After a day, the patient is prescribed an antibiotic and discharged from the hospital with a follow-up scheduled for a month later. Clinique Menara physicians monitor the patient for five years, during which blood tests are performed every three months to ensure that PSA levels are either stable or decreasing.
Fast, “one-and-done” HDR brachytherapy boost a winner at Clinique Menara
Beyond the clinical advantages of an HDR brachytherapy boost after EBRT, the advantage of limiting the treatment to a single fraction encouraged Dr. Ammor to adopt the technique.

“Not all of our prostate cancer patients are from Marrakesh, many of them live in the countryside, so it’s difficult for them to reach the clinic,” he says. “Reducing their therapy to one visit is definitely more convenient for these patients and, arguably, safer given the Covid-19 pandemic.”
Physicist Ait Ayoub adds that the speed of the Flexitron afterloader complements the single-fraction ease of the procedure.
“Irradiation is delivered in less than 30 minutes and in many cases half that time when the Flexitron source is newer,” he observes. “The source position is also controlled with millimetric accuracy, so the result is any toxicity to OAR is as low as reasonably achievable, and the optimization of the isodose and dosimetry after needle implantation is very accurate.”
Learn more about Elekta’s brachytherapy solutions.
References
- Ishiyama H, Kamitani N, Kawamura H, et al. Nationwide multi-institutional retrospective analysis of high-dose-rate brachytherapy combined with external beam radiotherapy for localized prostate cancer: An Asian Prostate HDR-BT Consortium. Brachytherapy 2017;16:503-10. [Crossref] [PubMed]
- Spratt DE, Zumsteg ZS, Ghadjar P, et al. Comparison of high-dose (86.4 Gy) IMRT vs combined brachytherapy plus IMRT for intermediate-risk prostate cancer. BJU Int 2014;114:360-7. [PubMed]
- Kishan AU, Shaikh T, Wang PC, et al. Clinical outcomes for patients with gleason score 9-10 prostate adenocarcinoma treated with radiotherapy or radical prostatectomy: a multi-institutional comparative analysis. Eur Urol 2017;71:766-73. [Crossref] [PubMed]