Belgian clinic enhances confidence with faster, easier end-to-end patient QA

Elekta Patient QA solutions help save time and improve quality of life for physicists at Grand Hôpital de Charleroi Gilly
Elekta Patient QA solutions not only enhance confidence in treatments at the radiation therapy department of Grand Hôpital de Charleroi Gilly, Belgium, but they also save time and improve the quality of life for their physicists. We asked medical physicist Michaël Del Re, MPE, Ph.D., to share his experiences.
Elekta: What patient QA requirements do you follow in your department?

Dr. Del Re: Patient QA measurements are not mandatory but highly recommended in Belgium. We follow the recommendations in Report NCS-24 of The Netherlands Commission on Radiation Dosimetry1.
Elekta: How did you perform patient QA previously, and what challenges did you have?
Dr. Del Re: Previously, we used a phantom-based method for pre-treatment QA. The challenge with this method was the time required to set up the detector and for the subsequent analysis (about 15 minutes before and 10 minutes after measurements). Because of this, we had to group pre-treatment QA measurements to avoid wasting too much time, which meant we didn’t have the flexibility to start new patients any day of the week. We needed a solution that would allow us to perform pre-treatment QA every day.
For in vivo dosimetry, we used diodes for our 3D-CRT treatments. This method was time consuming to set up for the radiation therapist and uncomfortable for patients because the diodes had to be attached to the patient’s skin with an adhesive. It also lacked accuracy and was not applicable for modulated treatments. We wanted a QA method that would check our end-to-end IMRT and VMAT workflows, including patient position, to ensure patients are treated correctly. About 60 percent of our treatments are VMAT, so it’s important for us to have an in vivo dosimetry method that is suitable for modulated treatments.
Complete patient QA suite of secondary check, pre-treatment check and in-vivo check
Elekta: When did you start to use the Elekta Patient QA solutions?
Dr. Del Re: We began using MU2net clinically in 2012, and then we started using EPIbeam and EPIgray clinically in 2016. We immediately saw the potential of EPIbeam and EPIgray to replace our pre-treatment QA method and to access in vivo dosimetry for our modulated treatments.
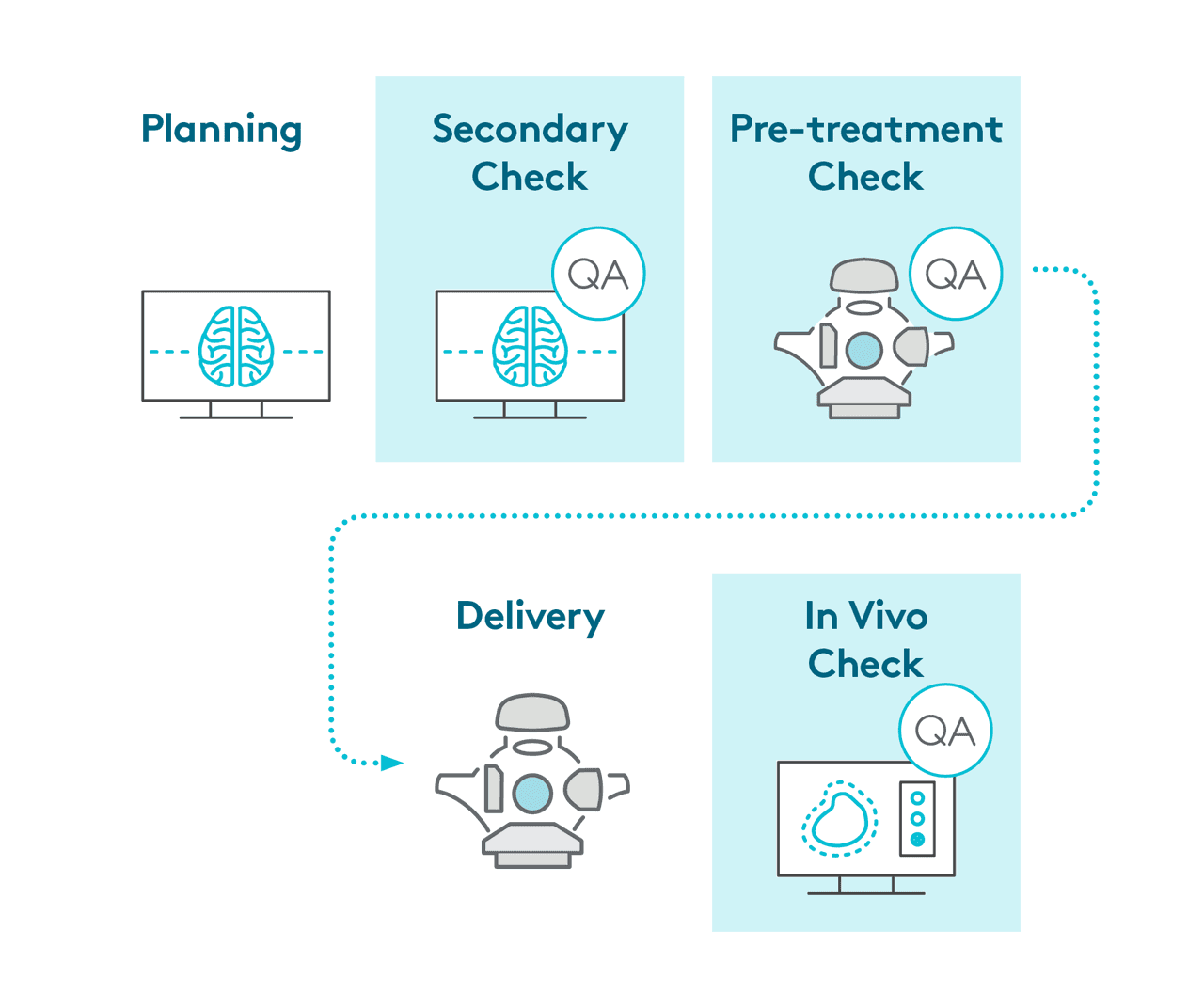
Manage physicist workload: Enable more delegation with automated workflows
Elekta: Please describe your patient QA workflow with the Elekta Patient QA solutions.
Dr. Del Re: With EPIbeam, we can measure a VMAT plan within just four minutes (the delivery time for 2 arcs) because all we need to do is open the EPID panel and launch the iView acquisition. Nothing else is required. Since there is no complicated detector set up, we can complete a pre-treatment QA measurement for a single patient any time there are five minutes free on a linac. It’s very fast–with EPIbeam. We have results in a few minutes.
We analyze the EPIbeam results as soon as possible after the measurement, and we use the software’s traffic light system, which is easy to follow. If it’s green, which is most of the time, we know everything is OK (within our tolerances) and we just save a pdf report in the patient’s file. If it’s red, we go deeper in the EPIbeam software to find the problem.
For in vivo dosimetry, the radiation therapist simply launches the EPIgray data acquisition, which occurs during treatment delivery without adding any time to the 15-minute treatment slot. EPIgray recalculates the dose for the whole patient with much better accuracy compared to our previous diode solution, giving us more confidence in our plans.
When an EPIgray measurement has been performed for a patient, the radiation therapist sends us a task in MOSAIQ® and we try to analyze the results within the hour. Again, we use the software’s traffic light system. If it’s green, we simply save a pdf report, and if it’s red we go deeper in the software to find the problem.
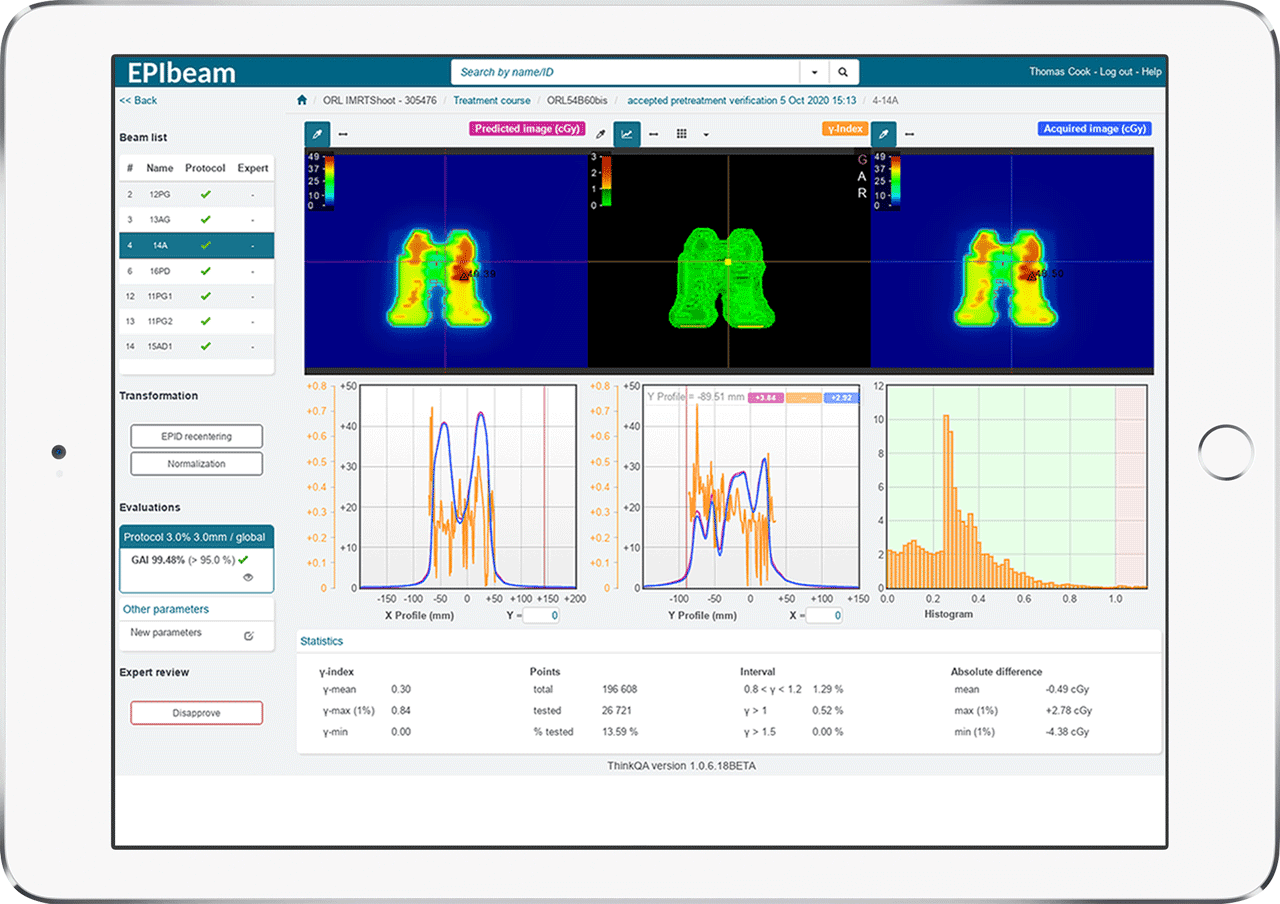
Unlock actionable insights: Focus on results with automated workflows, dose calculations and dose deviation alerts
Elekta: What difference have these solutions made to your workflow?
Dr. Del Re: MU2net provides a valuable double check of monitor units. It’s fast, automatic and will detect big errors in a plan.
EPIbeam saves us a lot of time and is really fast, with only three clicks to obtain the result. Previously, for pre-treatment QA, a physicist had to create a QA plan for calculating planar dose and compare this with the phantom detector measurements. They also had to set up the detector at the linac. This is not necessary with EPIbeam. The physicist simply exports the DICOM plan data to the EPIbeam server and launches the test. They can then look at the results back at their desk.
“EPIgray is more accurate than our old diode in vivo dosimetry technique and can be used for VMAT plans. It checks the entire workflow, including the patient, which is very important for us.“
In the past, the radiation therapist had to place a diode on the patient’s skin at the isocenter. We then received the diode reading from them, which we had to convert into dose–and we could only do this for 3D-CRT beams. With EPIgray, we just receive a notification that the iView images have been recorded. We then associate these images with the patient plan and the calculation starts automatically.
EPIgray has been received really positively by the radiation therapists because it is so easy for them; it doesn’t add any time to the treatment slot and it’s much more comfortable for the patient.
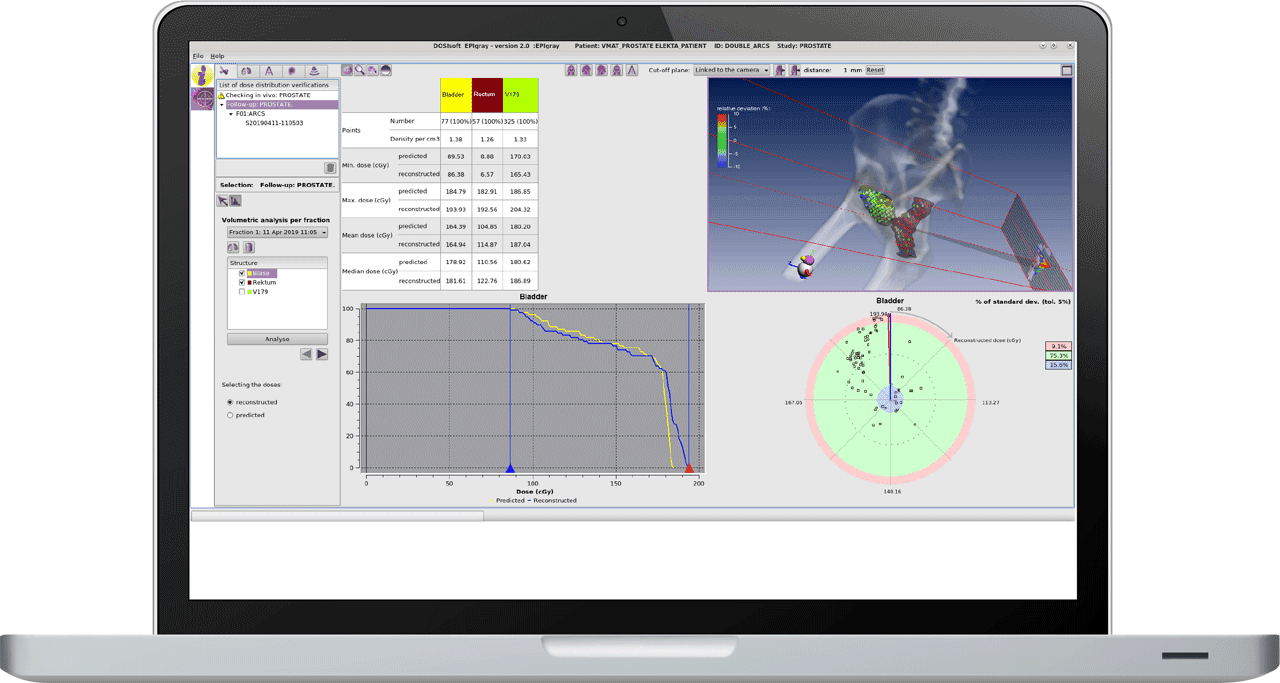
Gain confidence for advanced treatments with fast and efficient QA tests
Elekta: Have you experienced any other advantages with the Elekta Patient QA solutions?
Dr. Del Re: Another great benefit of EPIgray and EPIbeam is their accuracy for stereotactic beams. Phantom-based QA may not be optimal for very small fields because the detectors are usually spaced 5-10 mm apart. The increased resolution of the portal dosimetry panel offers tremendous accuracy for very small targets (such as brain metastases).
This is really important for us because we are treating more and more patients by stereotactic VMAT. Currently, about 20 percent of our VMAT treatments are stereotactic, and this is increasing. In such cases, the accuracy of the measured penumbra is crucial for checking the very high dose gradient between targets and OARs, requiring very good resolution. The iViewGT™ panel has a resolution of <0.3 mm, which is unbeatable compared to other phantom-based techniques. This gives us greater confidence in the accuracy of our stereotactic plans for very small targets.
Elekta: In summary, how does it benefit you to have the complete suite of Elekta Patient QA solutions?
Dr. Del Re: The real benefit is the freeing up of physicist time. We can check treatment quality faster than before thanks to these three solutions.
“The real benefit is the freeing up of physicist time. We can check treatment quality faster than before thanks to these three solutions.“
Now, physicists can spend more time on treatment planning and various other ongoing projects in the department, such as preparation for our move to a brand new hospital in two years’ time, which is really appreciated.
Since pre-treatment QA measurements no longer have to be grouped, the need for physicists to work after hours has also reduced. Being able to finish on time has improved the quality of life for physicists. EPIbeam, in particular, saves physicists 1-2 hours per week, which is a huge improvement compared to the situation 10 years ago when we frequently had to be onsite until 8 p.m.
And then you have peace of mind–if you have a quick MU check with MU2net, pre-treatment QA with EPIbeam, and in vivo dosimetry with EPIgray, and everything is within your tolerances, you can be confident that your treatments are correctly delivered.
Learn more about Elekta’s Patient QA solutions.
Reference
- Report 24 of the Netherlands Commission on Radiation Dosimetry. Code of practice for the quality assurance and control for Volumetric Modulated Arc Therapy. February 2015. https://doi.org/10.25030/ncs-024.
E058522





